Cataract FAQs
Cataracts are an opacity or clouding of the normally crystalline lens of the eye, caused by the natural aging process, metabolic changes, injury, various forms of radiation, toxic chemicals and certain drugs. The leading cause of vision loss among adults age 60 or older, cataracts impair vision, making everyday activities increasingly difficult.
There has been a rapid evolution in cataract treatment over the past few years, which translates to added patient benefits, including improved visual outcomes and faster recoveries.

Cataract Frequently Asked Questions
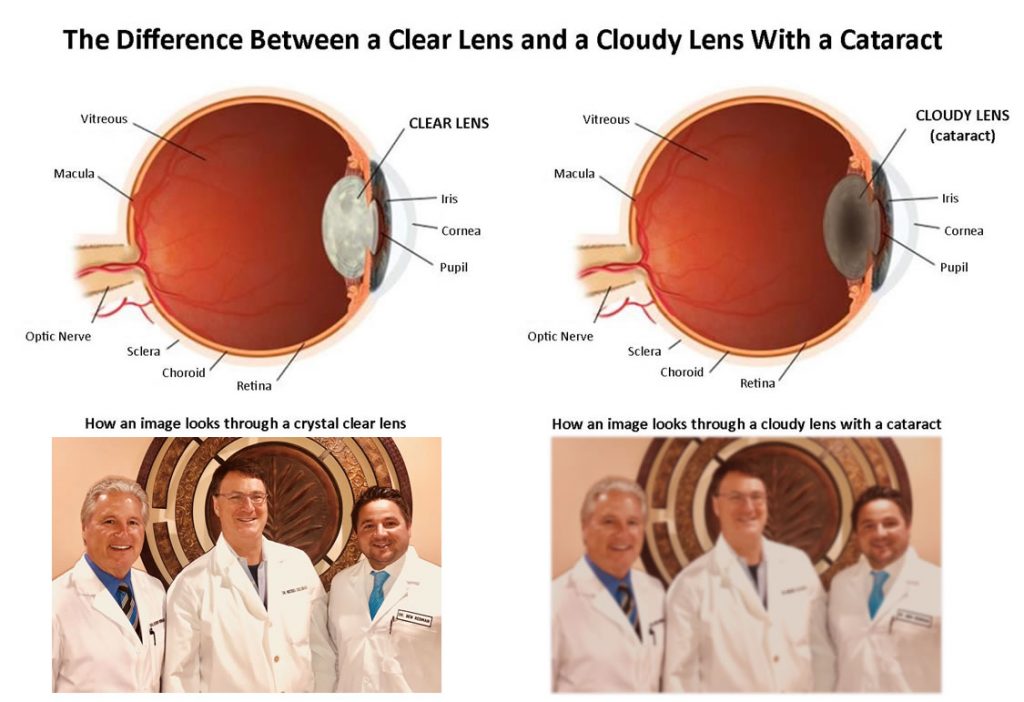
What is a cataract?
We all are born with a lens inside of each of our eyes. This lens is typically crystal clear, and we see through it like we would see through a clean, brand new window. As part of the natural aging process, the crystal clear lens inside of our eye will slowly lose its clarity and start to become cloudy or foggy. When this happens, patients will eventually begin to notice an overall decline in the quality of their vision—much like as if one were looking through an old, dirty window—however; this change is rarely sudden, it occurs slowly over many months to years, and many patients won’t even realize they have a cataract once they begin to develop.
What symptoms do cataracts cause?
Cataracts develop differently in many people, so not everyone with a cataract will have the same symptoms as the next person. Some people see just fine in daylight and can read with ease, but come night time, they struggle with their vision. Other people don’t notice issues with their night vision, instead their overall quality of vision becomes challenging, regardless of how bright or dark the room is. Some of the more common symptoms of cataracts include:
- Clouded, blurred or dim vision
- Difficulty with smaller print
- Increasing difficulty with vision at night
- Sensitivity to light and glare
- Need for brighter light for reading and other activities
- Seeing "halos" or “starbursts” around lights
- Frequent changes in eyeglass or contact lens prescription
- Fading or yellowing of colors
- Double vision in a single eye
*** Double vision isn’t always caused by a cataract—if you are experiencing double vision—you should call your eye doctor and talk to a technician or the doctor about your symptoms right away. They will help determine the appropriate time frame to get you seen for a thorough examination, as some conditions may need to be seen urgently. While this is rare, it is always best to call your eye doctors office to have them further advise.***
What causes cataracts?
Scientifically, cataracts are caused by a build-up of protein that clouds the eye’s lens, which can lead to blurred vision. According to the American Academy of Ophthalmology, this process tends to begin naturally between the ages of 50 and 70. Other health issues, medications, previous eye surgery, or trauma can also cause a cataract to develop. Diabetic patients are more likely to develop cataracts earlier in life, especially if their blood sugars that are harder to manage. Patients that use oral steroid medications on a frequent basis or in high doses can also develop cataracts as a possible side effect of the medication.
Preventing cataracts...
Realistically, we cannot prevent cataracts—as long as we all live long enough, we will all develop some degree of a cataract at some point in our lives. However; developing certain habits and adopting certain lifestyle changes can delay or potentially slow the development of a cataract. These include:
- Wear Sunglasses with UV Protection. A recent John Hopkins study concluded with ample evidence that years of chronic sunlight exposure increases your risk of cataracts. Wearing sunglasses with UV protection is one of the simplest and most cost effective measures you can take to protect your eyes from ultraviolet radiation emitted from the sun to protect your eyes. Wearing a brimmed hat to block the sun’s rays, in conjunction with UV protection sunglasses, will also give your eyes added protection.
- Eat a diet rich in beneficial nutrients. We’ve all heard about carrots being good for your eyes… but the truth is that yellow or dark-green leafy vegetables are the BEST. Yellow and dark-green leafy vegetables contain the antioxidants lutein and zeaxanthin, which are amazing antioxidants specifically for eye health! Studies have demonstrated how a diet rich in omega-3’s (found in oily fish such as salmon, sardines, and even flaxseed) had an impact in delaying the development and progression of cataracts. But don’t stop eating those carrots… eating foods high in antioxidants, such as beta-carotene, selenium, and vitamins C and E, were also proven to help delay cataract development.
- Stop Smoking. Smoking doubles your chances of developing cataracts and the risk continues to grow based on how much you smoke.
- If You Are Diabetic, Control Your Sugars. An increase in blood sugar (glucose) also affects the fluid inside of the eye, which is called the aqueous humor. This fluid surrounds the lens inside of the eye. When glucose levels rise the in blood, they also rise in the aqueous, which causes the lens to swell, leading to a shift in the vision. Over time, this process will result in the production of added proteins inside of the eye and eventually cause the lens to become less clear and more opaque (i.e. cataracts begin to develop).
- Wear Safety Glasses. When you’re out and about engaging in the tasks of everyday life, there are some activities that protective eyewear should ALWAYS be worn for. This includes activities such as mowing the lawn, weed-whacking, cutting firewood, using ratchet or tow straps, playing baseball and even fishing. Basically, any activity where objects have the potential to make impact with you at a high speed is the right circumstances to wear some form of safety glasses. If one of your eyes gets hit with the tip of a fishing pole during a cast or a tow strap snaps and hits your eye—you may not always have obvious trauma to your eye other than the sensation of it being tender. However, hidden inflammation within the eye can cause bigger issues that will need to be addressed—including the development of a cataract.
I have a cataract, what do I do?
When glasses and good lighting just aren’t enough to function as you would like, it’s time to consider cataract surgery. There are no vitamins or eye drops that can reverse cataracts or make your vision better. The only solution is cataract surgery, but not to worry, cataract surgery is not nearly as invasive as it was decades ago—today, it is a procedure that has you back at home within just a couple of hours and the surgery time itself is typically less than 21 minutes (according to national averages published by the American Academy of Ophthalmology).
Cataract Surgery
Cataract surgery is performed by a well-trained, highly skilled eye surgeon called an ophthalmologist. The surgeon will perform the surgery under a high powered microscope so that they have an excellent view and are able to see clearly, and be very precise. Most patients prefer some relaxing medication prior to the surgery, but the procedure is so non-invasive thanks to modern technology it can be done without any sedation or relaxing medication at all! An anesthetic eye drop (or occasionally, an injection) is used during the procedure which makes the procedure painless and the patient is free of any discomfort. The surgeon will gently place a special instrument along your eyelids to prevent blinking during the procedure, while a surgical assistant will keep the eye hydrated with sterile, surgical grade saline designed for use in the eye during surgery and then the surgery will begin.
The surgeon will make a very tiny, almost microscopic incision, near where the white part of the eye and the colored part of the eye meet which is called the limbus. Through this incision the surgeon gains access to the cataract by using a tiny instrument called a phaco probe. The probe uses a very gentle ultrasonic power and gently breaks up the cataract into smaller pieces. Once the cataract is broken up into pieces, the surgeon is then able to gently suction out the pieces until all of the cataract is gone. Once the cataract is completely removed, the surgeon will replace that lens with a new and clear lens in order for you to see well again. This new lens has been determined based on special measurements that were taken prior to surgery and has been “loaded” into a special tool, ready to implant in the eye where the old lens was. Once that lens is inserted into the eye, the surgery is complete. The surgical staff will take over and bring you to recovery where you will be prepared for discharge.
The procedure itself takes less than 15 minutes! However, patients can expect to be at the surgery center for 1.5-2 hours for the entire process, from check-in to check out. There are very few restrictions following surgery which include avoiding hot tubs, swimming, strenuous activities such as golfing, shoveling and heavy lifting for about 1 week following surgery. You will need a driver for the day of surgery, but most patients are able to begin driving again the following day.
Cataract surgery is considered one of the most popular and highly successful procedures, with improved vision occurring in over 90 percent of cases. In fact, a study by the American Society of Cataract and Refractive Surgery recently reported that more than 98 percent of cataract patients had their vision successfully improved following surgery. Many patients report vision that is even better than before they developed cataracts. Results are permanent and so once removed, cataracts will not reoccur.
Implant and cataract procedure options
Cataract surgeons offer premium implant lenses that select candidates can consider. Cataract surgery in itself tends to offer patients less dependence on glasses or contacts afterwards, but patients can still expect, at a minimum, to need correction for their near vision and to correct astigmatism—if it is present—after surgery. For patients that qualify, and want to invest more into their vision as a means of being even less dependent on corrective wear, premium implant lenses and/or laser may be discussed and considered.
MULTIFOCAL IMPLANT: A multifocal implant lens is one option that may be discussed prior to surgery. This is an implant lens designed to help patients see at various ranges—distance (road signs), intermediate (speedometer), and near (reading a book), at a higher quality than a standard implant lens would. It acts much like a bifocal or trifocal in your glasses would work, without obvious lines to look past as the implant gradually adjusts the power for various ranges. Keep in mind, this is still an artificial device and artificial devices are never the same as when we had a well-functioning natural device (i.e. natural, clear lens before cataracts).
TORIC IMPLANT: A toric implant lens is also an option for patients that have a more clinical amount of astigmatism. An astigmatism has nothing to do with a cataract, instead, an astigmatism has to do with the shape of the cornea (the window on the front surface of our eye) and how light focuses inside of the eye. Toric implant lenses are quite unique because they have the ability to correct visual disruption caused by astigmatism without changing the shape of the cornea. This makes for a higher success in the quality of a patients vision after cataract surgery and allows patients to see much sharper at a distance with little correction after surgery. It is important to note that toric implants correct for sharper distance vision, but reading glasses may still be necessary at a minimum.
LASER: Laser assisted cataract surgery is a popular option and can be done using traditional or premium lens implant options. With laser-assisted cataract surgery, a camera-like ultrasound imaging device is placed over your eye to map the surface of the eye and gather information about the lens. The device sends detailed information to a computer that programs the laser for the exact location, size and depth of the incisions. The surgeon uses the laser to make the incision and gain access to the cataract. Energy from the laser may also be used to soften the cataract. Then the ultrasound probe used in traditional cataract surgery is used to break the lens into pieces and suction them out of the eye. Using a laser to do cataract surgery allows the surgeon to make very precise incisions in less time. It can improve accuracy and consistency in the surgical steps. In some cases, laser-assisted cataract surgery can provide a higher degree of correction for a refractive error, such as astigmatism, than traditional cataract surgery. Again, as with traditional and toric implants, reading glasses may still be necessary.